Stopping Gingivitis
Gingivitis is one of Canada’s most common oral diseases. Yet, gingivitis is preventable and can be treated when detected early. Preventing gingivitis is a team effort. Regular dental exams and at-home oral hygiene can help your oral health and stop the development of gingivitis.
Learn how to protect your gums and oral health with our team at Otara Dental.
What Is Gingivitis?
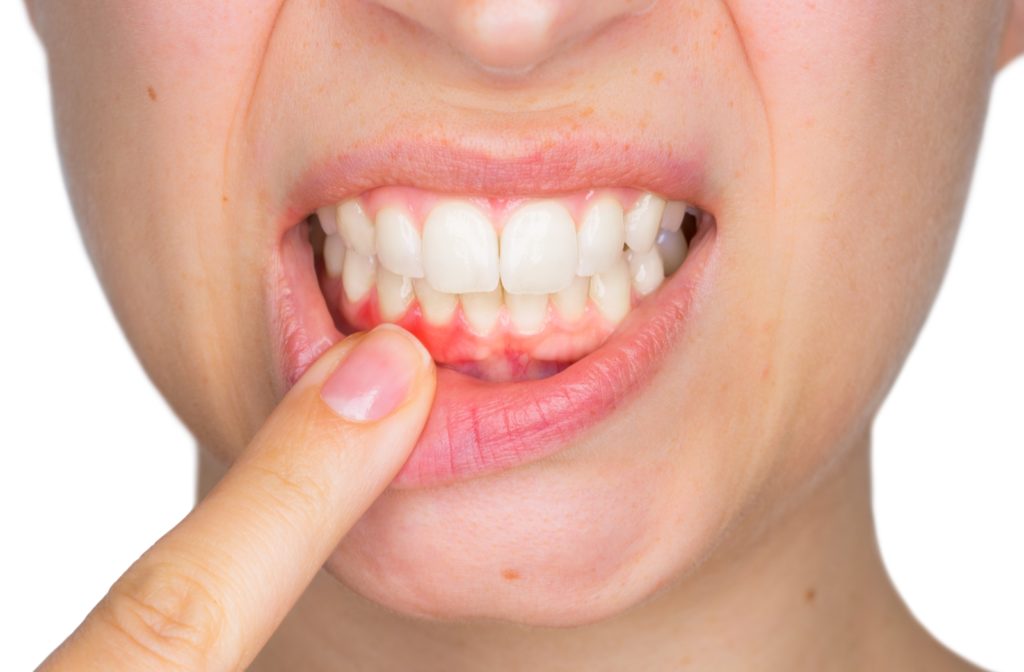
Gingivitis is inflammation of the gums alone. When gingivitis is left untreated it will develop into periodontal disease, also known as severe gum disease . The oral condition is either plaque-induced or non-plaque-induced. However, both causes can result in severe disease that may cause tooth loss.
The most common form of gingivitis is a chronic bacterial infection affecting 16 million Canadians caused by plaque around the teeth and gums.
When untreated, gingivitis can weaken gums and teeth, causing irritated gums, tooth loss, bleeding gums, bone loss and attachment loss.
What Causes Gingivitis?
Gingivitis is caused when dental plaque builds on teeth and the gingiva (gums). Dental plaque is a sticky substance that feeds on the sugars and food debris leftover after eating and drinking. It contains harmful bacteria, chemicals, and acids.
When plaque isn’t removed regularly, it can accumulate, causing damage to teeth, gums, and bone. The damage is what commonly causes tooth decay or gingivitis. Eventually, the clear, sticky substance hardens into a rough substance, called tartar or calculus, which you cannot remove with at-home brushing and flossing.
If the infection progresses, it can lead to a more advanced form of gum disease, periodontitis, which cannot be reversed.
Other Causes of Gingivitis
Although plaque is the most significant cause of gum disease, other risks can cause gingivitis, including:
- Family history of gum disease
- Chronic conditions (diabetes, HIV, cancer)
- Hormonal changes
- Medications
- Smoking
Aging can also increase the risk of gum disease, as the cells renew more slowly and gums recede. Although slight, the increase in space between your gums and teeth creates more opportunities for bacteria to build up and cause inflammation.
Symptoms of Gingivitis
The primary symptom of gingivitis is gum inflammation, but it can present in multiple ways. Therefore, knowing the difference between developing gum disease or a temporary reaction or injury can be challenging without professional knowledge.
For example, if you skip flossing most days, you might notice some bleeding or soreness when you start flossing again. Yet, bleeding and soreness are symptoms of gum disease. So how can you tell the difference?
Your dentist can assess your dental health for gingivitis at your regular dental exam and cleaning. If there are warning signs, your dentist will share their assessment and advise what you should do next.
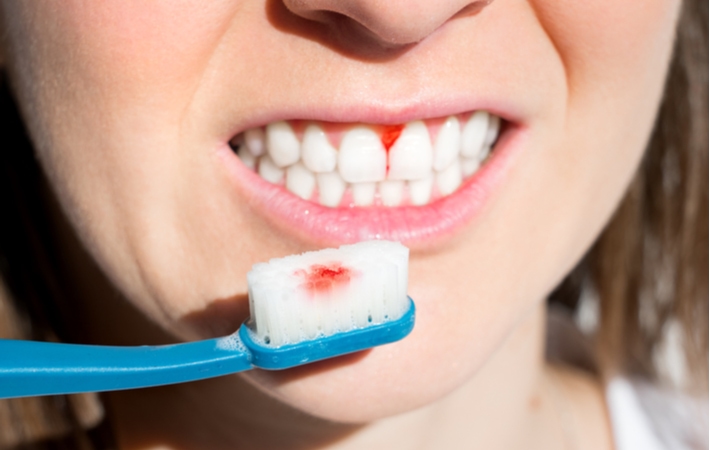
If you’re in-between visits and you’re not sure about what to watch for, here are some symptoms warning gingivitis may be developing:
- Bleeding gums
- Receding gums
- Changing bite
- Metallic taste
- Tooth sensitivity
- Red or tender gums
- Loose/separating teeth
- Dentures misfitting
- Gum colour change
- Bad taste in your mouth
- Persistent bad breath
- Shiny, puffy, or swollen gums
- Pus between teeth or gums
You may not experience all possible symptoms. The less you experience, the better, as symptoms can worsen as gum disease progresses. It’s best to check in with your dentist as soon as possible if you notice even minor symptoms.
Methods of Reversing Gingivitis
Gingivitis can be reversed, however, if left untreated the resulting periodontitis is not reversible. It is therefore essential to practice good oral hygiene to prevent gingivitis or treat it before it worsens.
There are multiple options for treating and reversing gingivitis, depending on the stage of the disease.
During the earliest stages of gum disease, deep cleaning methods, including teeth scaling, are implemented by a dentist to remove difficult plaque and tartar. Your dentist may also prescribe antiseptic mouthwash, antibacterial toothpaste, or oral antibiotics.
For treatment of severe gum disease you may require surgery after tissue or bone loss. Some surgery options include a gum graft, dental bone graft, or flap surgery.
Your dentist can perform or prescribe some of the methods used for gingivitis or advanced gum disease. However, in severe cases some patients need the help of a gum specialist known as a periodontist.
You Can Prevent Gingivitis
The best way to stop gingivitis is to prevent it. Visiting your dentist regularly for teeth cleanings can help prevent plaque buildup, and it’s the only way to remove dental tartar.
You can also practice oral hygiene at home: Here are tips for protecting your oral health and preventing gingivitis:
- Brushing twice daily for 2–3 minutes
- Flossing daily, both sides of every tooth
- Reducing sugar and eating a balanced diet
- Avoiding oral health risk factors
- Reducing alcohol consumption
- Stopping smoking or vaping
Partner with Your Dentist for Oral Health
Maintaining your dental health is part of your every day, but it’s not a challenge you need to face alone. At Otara Dental, we’re your oral health partners. We can help your teeth and gums fight plaque and gingivitis so you can enjoy a healthy smile.
Contact our team and request an appointment for compassionate dental care.